The Suitcase and The Silence: Remembering Dr. Abdul Rahman and Dr. E.K. Ummer
By Dr Venugopalan P P
There are wounds that time heals, and then there are voids that remain largely unfilled—spaces once occupied by giants whose shadows gave us shade. As I look back at the history of healthcare in Kerala, specifically the rise of critical care and emergency medicine, two faces emerge from the mist of memory. They were my mentors, my guides, and the architects of a medical revolution.
Sadly, they were also the casualties of a war we fought in PPE kits and makeshift ICUs. This is the story of Dr. Abdul Rahman and Dr. E.K. Ummer—and the "what ifs" that still haunt the silence of the aftermath.
The Visionary: Dr. Abdul Rahman
To call Dr. Abdul Rahman a physician is an understatement. He was a force of nature. Long before corporate healthcare took root, he was redefining what it meant to serve a community.
In the 1990s, in the semi-rural setting of Korambayil Hospital, Manjeri (Malappuram District), Dr. Rahman was already ahead of his time. He didn’t just treat patients; he built systems. He established a critical care setup in Manjeri that saved countless lives and initiated basic training to empower junior doctors and nurses in casualty management.
His heart, however, beat for the marginalized. He was deeply embedded in charitable trusts supporting educationally backward Muslim communities and was a pillar of the palliative care movement in Malappuram.
The "Triple A" Victory
When Aster MIMS (Calicut) began its journey in 2002 as the first corporate hospital in Kerala, Dr. Rahman was its heartbeat. He was the best companion to the passionate Medical Director, Dr. Abdulla Cherayakkat. Together with the Chairman Dr. Azad Moopen, they formed the "Triple A"—Abdulla, Abdul Rahman, and Azad. This trio was the engine behind the phenomenal, historic growth of Aster MIMS in its first 15 years.
Dr. Rahman was the "live wire" who brought the Indian Society of Critical Care Medicine (ISCCM) to Calicut in the early 2000s. But for me, his legacy is personal. He was the driving force behind the MIMS School of Resuscitation. Because of his vision and support, I had the fortune of serving as the Director of this school for nearly a decade, overseeing massive public BLS training initiatives.
He was a mentor who didn’t just lead; he pushed. He supported me in launching the first Mobile ICU in Kerala (2005) and the first nurse-based EMS course at Aster. He was a true entrepreneur, administrator, and born leader.
Most poignantly, Dr. Rahman was a man of ethics. He had crystal-clear concepts regarding End of Life Care. He was a staunch advocate for DNR (Do Not Resuscitate) status in futile cases and was vocal against placing patients without medical hope on advanced ventilation.
The Strategist: Dr. E.K. Ummer
If Dr. Rahman was the architect of critical care, Dr. E.K. Ummer was the strategist of disaster management. A renowned General Practitioner from Nilambur and a senior leader of the Indian Medical Association (IMA), Dr. Ummer was a man of immense stature—State President of IMA, National leader in the IMA Disaster Management Cell, and a dedicated Rotarian.
But to me, he was a friend whose hospitality was unparalleled. I remember the many visits to his home in Nilambur, surrounded by his love and affection.
We worked side-by-side during his tenure as IMA State President. He was the wind beneath my wings during the formation of the ANGELS network (Active Network Group of Emergency Life Support). As an office bearer of the Angels Malappuram unit, he was instrumental in creating a cohesive ambulance network across the district. He was a strategist, a mentor, and above all, a great human being.
The Arrival of the Suitcase
The tragedy of their departure is marked by an eerie, heartbreaking parallel.
It was the tail end of the first COVID phase. One morning, Dr. Abdul Rahman walked into the Emergency Department. He had come straight from the airport, suitcase in hand, returning from the Middle East after visiting his daughter.
"I am suspecting I have COVID," he told me.
We did the initial evaluation. He was admitted to the Medical ICU. That was the last time I saw him as the man I knew. He deteriorated, requested a discharge to IQRA Hospital, and later suffered a stroke. He was shifted to Meitra Hospital and placed on a ventilator.
The irony broke my heart. The man who spent a lifetime advocating against futile ventilation for patients with no hope ended his journey on a machine he viewed with such ethical caution. He succumbed to the virus—a massive loss for the medical fraternity.
Shortly after, the nightmare repeated itself.
One morning, Dr. E.K. Ummer walked into the ED. Like Dr. Rahman, he was carrying a suitcase.
"I think I have COVID," he said, his voice laced with anxiety.
I took him to the acute care area. His SpO2 was already beginning to drop. We started oxygen, but by evening, he was shifted to the ICU on the second floor. It was the early, brutal phase of the second wave. He deteriorated rapidly, was intubated, and very shortly after, he too succumbed.
The Shock and The Regret
Writing this now, I am still gripped by the shock of those dark days. My favorite mentors were killed by a virus we were struggling to understand. I still have bad dreams of the second wave, the days I spent running a 100-bed makeshift COVID ICU, fighting a tide that seemed unstoppable.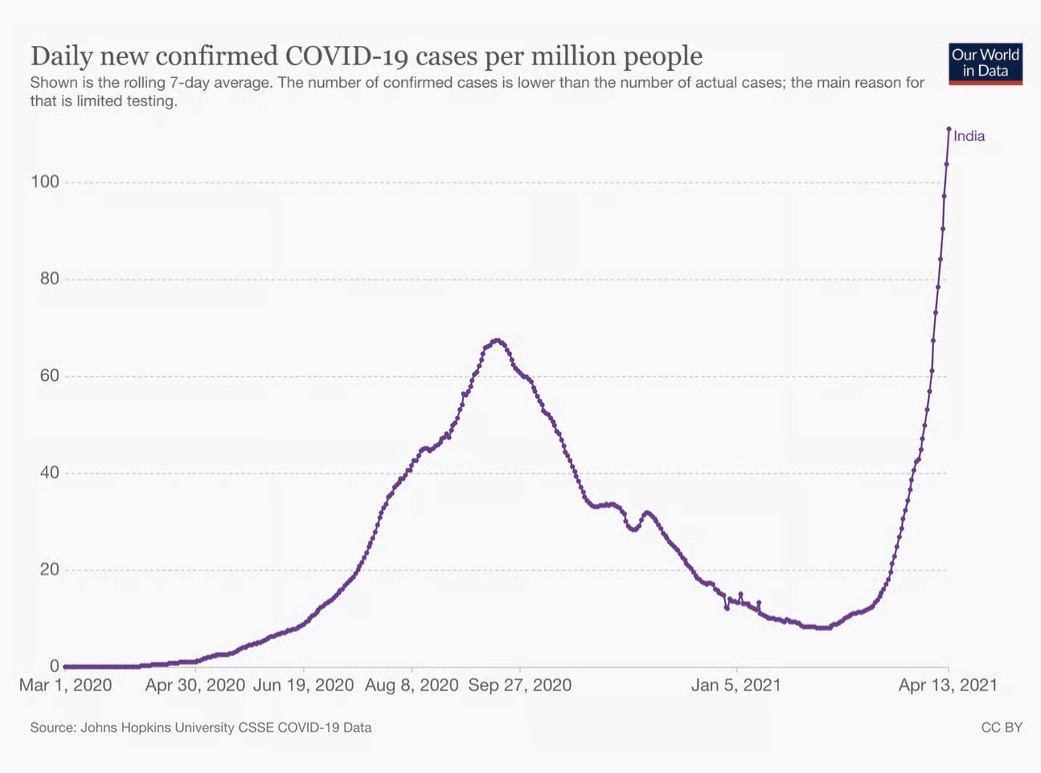
But the bitterest pill is the timing.
In the later part of the second phase, a magical drug entered the market: Monoclonal Antibodies. With this drug, I was personally able to save more than 200 elderly, severely compromised, and co-morbid patients from death.
It is a thought that haunts me: If only this drug had been available a few months earlier.
I strongly believe that if Dr. Rahman and Dr. Ummer had access to Monoclonal antibodies, they would have benefited. They would likely still be here today—guiding us, scolding us, and leading us.
We lost two pillars of Kerala’s medical history to the timing of fate. But while they are gone, the systems they built—the critical care units, the ambulance networks, the resuscitation schools—remain. They live on in every life saved by the infrastructure they helped create.
Rest in peace, my mentors. You are missed, but never forgotten.





 (Human Insulin - helped me overcome allergy and insulin resistance )
(Human Insulin - helped me overcome allergy and insulin resistance )